The Pharmacy Counter Problem: How Waltz Health is Meeting the Moment

The prescription experience remains one of the most fragmented and confusing touchpoints in healthcare. Consumers are facing a system that hasn’t kept pace with their expectations. Waltz Health is meeting the moment with innovative solutions that support smarter prescription decisions and improve access at scale.
New data from Waltz Health’s consumer surveys, conducted through Suzy, shows that while most individuals report general satisfaction with their prescriptions, many struggle to understand costs, coverage, and available options. These challenges are especially pronounced among those new-to-therapy, managing chronic conditions like diabetes, or filling medications at specialty pharmacies.
A System Misaligned With Consumer Needs
We see this disconnect play out every day. According to KFF, prescription drugs account for about 10% of total U.S. healthcare spending, yet they shape a much larger part of the consumer’s healthcare journey. For patients managing chronic therapies, the pharmacy is a recurring experience, often filled with confusion and frustration.
One GLP-1 patient told us she had to contact her insurer and pharmacy multiple times to clarify coverage. Another abandoned treatment altogether after receiving conflicting answers about her medication. These experiences are emblematic of a system where access, price, and communication remain out of sync. The need for an integrated, transparent solution is more urgent than ever.

What the Data Tells Us
These aren’t isolated stories—they’re data-backed signals of a broader problem. We surveyed 1,491 consumers using retail, specialty, or GLP-1 medications. Here’s what they shared:
49% of GLP-1 users and 39% of specialty users always knew what they would pay before picking up a prescription.
Only 27% of GLP-1 users and 21% of retail users said it was easy to find ways to save.
43% of retail consumers and 34% of specialty users were surprised by the cost of their prescription in the past year.
Between 30% – 40% across all groups said they delayed care, switched pharmacies, or stopped taking a medication because of cost or coverage.
These numbers reveal a deeper issue. People want to make informed decisions about their prescriptions, but the system continues to put up barriers.
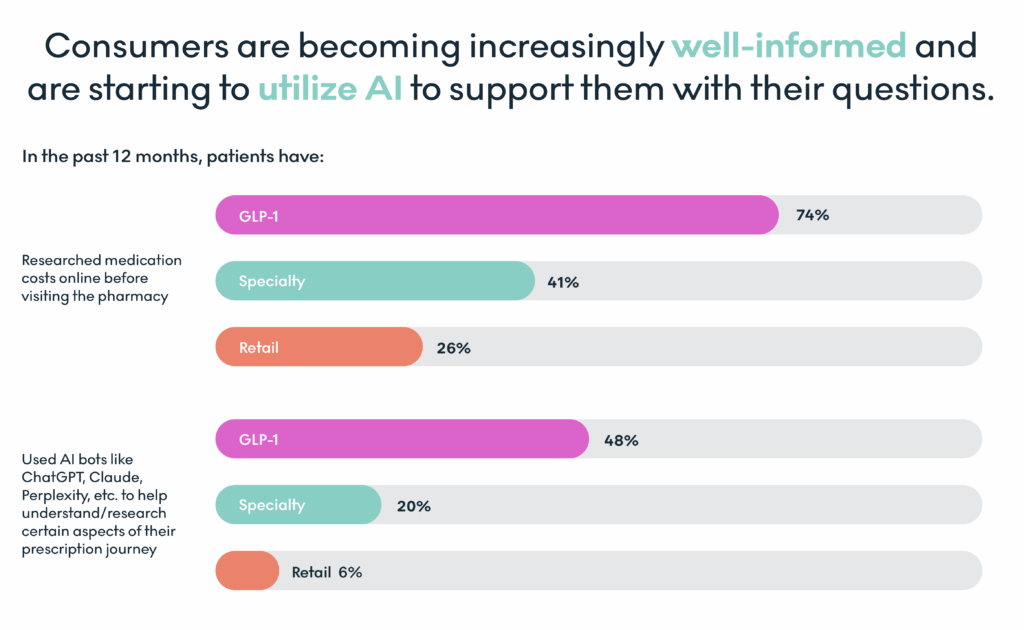
Patients Are Doing the Heavy Lifting
Consumers aren’t standing still. They’re researching prices, asking more questions, and actively seeking clarity. 74% of GLP-1 users looked up prices online before filling a prescription. Over half asked their provider or pharmacist about alternatives. Nearly half used AI tools like ChatGPT or Claude to understand coverage, side effects, or benefits. That’s a significant lift for patients trying to get the care they need.
These numbers highlight a fundamental shift: patients are acting more like healthcare consumers than ever before, and they’re hungry for clear, consistent information that helps them make better decisions.
Meeting Expectations with Smarter Solutions
This shift in behavior is part of a larger trend: the prescription experience is becoming more consumer-driven. At the same time, confidence in traditional players like health plans and providers is slipping. According to Forrester, only 56% of Americans trust their insurer, and two-thirds say no source stands out as most trustworthy.
Many now turn to social media and peers for answers, with younger adults reporting that online content strongly influences their health decisions. These dynamics increase pressure on the healthcare system to provide clearer, more reliable information and tools that people can trust.
Waltz Health is reducing that burden. Our technology helps payers, PBMs, and providers deliver an experience that’s simpler, faster, and easier to rely on. We’re helping health plans surface cost-saving options, reduce surprise bills, and improve experience and adherence by giving members more clarity at every step.
As more consumers expect the ease and transparency they’re used to in other industries, our tools are designed to help healthcare catch up. Waltz is uniquely positioned to support patients and partners in the pursuit of better experiences through greater empowerment, transparency, and saving.
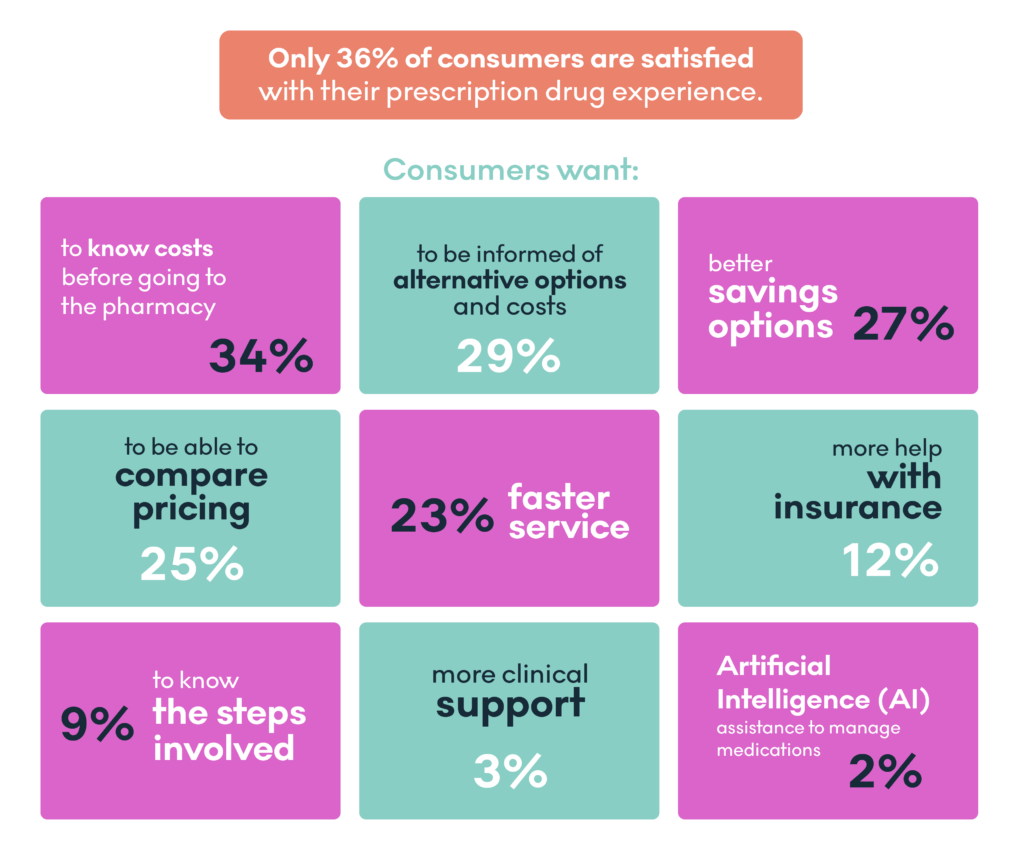
How Waltz Supports Better Decisions
At Waltz Health, we believe that to disrupt healthcare, we need to empower consumers with informed and timely knowledge—while removing unnecessary friction in their prescription care experience. That belief shapes how we build, design, and deploy our tools.
Marketplace Search gives consumers clear pricing across a marketplace of discount programs and cash prices. It can be integrated into health plan, PBM, and pharmacy portals and makes it easier for consumers to find the best cost option for their prescription.
Marketplace Search for Payers simplifies savings by embedding them directly into the insurance benefit – no external coupons or third-party tools required. Health plans and PBMs using this product report increased member engagement and streamlined operations.
Waltz Connect for Specialty and GLP1s offer real-time support for consumers navigating the specialty and high-cost pharmacy experience. These tools improve cost visibility, coordinate pharmacy access, and offer clear communication throughout the process. They help reduce delays, improve turnaround times, and keep patients on therapy.
Results That Raise the Bar
The results speak for themselves. According to Retently, the average Net Promoter Score (NPS) in healthcare hovers around 34, while retail typically reaches around 65, and financial services average about 62. Waltz Health’s NPS? 87.
This figure reflects more than satisfaction—it shows real progress in solving persistent friction points for consumers. We’re not just improving the prescription experience; we’re creating a smarter, more cohesive system that serves patients and health plans alike. It’s clear that the future of pharmacy engagement is driven by access to information, smarter tools, and a renewed focus on patient experience.
Contact Waltz to learn more.

Yi Gu
SVP, Consumer Engagement

